

PCOS (Polycystic Ovary Syndrome) is a common hormonal condition affecting many women today.
For many, it doesn’t appear suddenly; it starts with small, often ignored changes like irregular periods, acne that doesn’t settle, or gradual weight gain despite no major lifestyle changes.
Because these symptoms don’t always seem connected, PCOS is often recognised later than it should be. Understanding these early patterns can make a significant difference in how effectively the condition is managed.
PCOS is a hormonal and metabolic condition that affects ovulation and increases androgen (male hormone) levels in women.
It is typically identified when there are irregular menstrual cycles, visible signs of hormonal imbalance such as acne or excess hair growth, or polycystic ovaries on ultrasound.
What makes PCOS complex is that it does not present the same way in everyone, which is why it is often overlooked in the early stages.
The symptoms of PCOS often develop gradually and may not seem connected at first, which is why many women don’t immediately recognise the pattern.
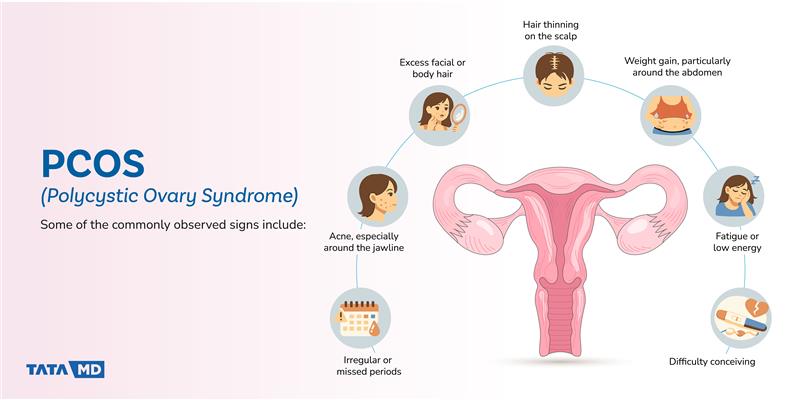
Some of the commonly observed signs include:
When multiple symptoms appear together over time, it may indicate an underlying hormonal imbalance that needs attention.
PCOS develops due to a combination of factors rather than a single cause.
One of the most common contributors is insulin resistance, where higher insulin levels affect hormone balance and ovulation. Hormonal imbalances involving reproductive hormones also play a key role.
In addition, genetic factors can increase the likelihood of developing PCOS. Lifestyle factors such as stress, poor sleep, and chronic inflammation may further influence how symptoms appear and progress over time.
PCOD and PCOS are often used interchangeably, but they are not the same.
PCOD is generally considered a milder condition related to the ovaries, while PCOS is a broader hormonal and metabolic disorder that can impact long-term health.
Understanding this distinction is important, as PCOS usually requires a more structured and long-term approach to management.
Diagnosing PCOS involves understanding both symptoms and underlying factors.
Doctors may recommend a combination of tests, including hormonal blood tests, glucose and insulin levels, thyroid function tests, and a pelvic ultrasound. These are supported by clinical evaluation to arrive at an accurate diagnosis.
Since symptoms can overlap with other conditions, diagnosis is based on identifying a pattern rather than relying on a single test.
Managing PCOS is not about short-term fixes. It requires a consistent and personalised approach that focuses on long-term balance.
Treatment may involve medical support where required, especially to regulate cycles or manage hormone levels. At the same time, nutrition plays a central role, particularly in improving insulin sensitivity.
Lifestyle factors such as regular physical activity, adequate sleep, and stress management are equally important. Over time, regular monitoring helps in understanding how the body responds and allows adjustments to the approach.
A structured and consistent plan is key to managing PCOS effectively.
Diet plays a central role in managing PCOS, especially when insulin resistance is present.
A balanced approach that includes fibre-rich foods, adequate protein, whole grains, and healthy fats can support hormonal balance. Reducing processed foods and excess sugar intake can help improve symptoms gradually.
Small, consistent changes in diet often lead to better long-term outcomes.
PCOS cannot be permanently cured, but it can be managed effectively with the right approach.
With consistent care, menstrual cycles can become more regular, symptoms can improve, and overall health outcomes can be better.
The focus is not on quick fixes, but on long-term management and stability.
PCOS is one of the common causes of irregular ovulation, which can affect fertility.
However, with proper management, ovulation can improve and the chances of conception can increase. Early identification and intervention often make a significant difference in outcomes.
If you notice ongoing irregular periods, persistent skin or hair-related changes, or difficulty conceiving, it may be helpful to seek medical guidance.
Early evaluation helps in identifying the underlying cause and starting the right approach at the right time.
If you are experiencing symptoms related to PCOS and are unsure about the next steps, a timely consultation can help you understand your condition and plan the right approach for management.